Search
Find a Physician
What is Joint Preservation? An Alternative to Joint Replacement

Medically Reviewed by
Ashley Bassett, MDBlog
Apr 17, 2026
Joint replacement surgery often sounds intimidating. Many people immediately picture long recovery periods, implants, and permanent changes to the body. That’s why patients frequently ask about joint preservation and whether it can help them avoid major surgery while still relieving pain and restoring mobility.
So, what is joint preservation? The idea behind it is to protect the joint's natural structure rather than replace it. Doctors look for ways to repair cartilage, improve alignment, or stimulate healing so the joint can function properly again without artificial components.
For many patients, this approach offers hope. In the right circumstances, preserving a joint can reduce pain, improve movement, and delay or even eliminate the need for replacement surgery. Understanding when these techniques work best helps patients make smarter decisions about long-term joint health.
What Does Preserved Joint Spaces Mean?
When doctors evaluate joint damage, they often look closely at the space between bones on imaging scans. If cartilage is healthy, it keeps the bones separated and allows smooth movement. Maintaining that gap is critical for long-term function.
Radiologists often refer to preserved joint spaces on X-ray when the cartilage between bones remains intact. This usually indicates that the joint still has structural integrity and that joint replacement may not be necessary yet.
The preservation of joint space becomes an important indicator for treatment planning. If the cartilage layer still provides cushioning, physicians may recommend conservative strategies designed to protect the joint rather than replace it.
This is one of the situations where patients begin asking what joint preservation is and how it applies to their condition. When the joint still has usable cartilage and reasonable alignment, preserving the natural joint becomes a realistic medical goal.
Maintaining preserved joint spaces often involves a combination of lifestyle changes, physical therapy, and targeted medical procedures. The goal is simple: reduce stress on the joint and protect the remaining cartilage.
What Joint Preservation Treatments Are Available?
Doctors use a wide range of joint preservation treatments depending on the joint involved, the level of damage, and the patient’s activity level. Many of these treatments focus on improving the joint environment so the body can heal itself.
Some approaches aim to restore cartilage or stimulate new tissue growth. Others correct structural problems that cause abnormal pressure inside the joint. The overall objective is to maintain mobility while preventing further degeneration.
Common joint preservation treatments include:
- Cartilage repair procedures
- Osteotomy to correct joint alignment
- Arthroscopic joint cleanup procedures
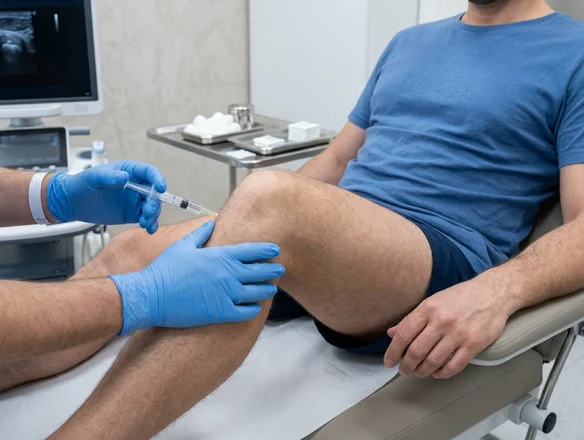
- Regenerative injections such as platelet-rich plasma
One advanced cartilage repair option is the MACI procedure (Matrix-Induced Autologous Chondrocyte Implantation). This treatment uses a patient’s own cartilage cells, which are grown in a laboratory, placed onto a collagen membrane, and then implanted into the damaged area of the joint. The goal is to regenerate cartilage and restore the joint surface, making it a promising option for patients with localized cartilage damage who want to preserve their natural joint.
Physical rehabilitation also plays a major role. A structured joint therapy program strengthens surrounding muscles and improves stability, which helps reduce pressure on the joint surface.
Doctors often recommend lifestyle adjustments alongside medical treatments. Weight management, activity modification, and muscle strengthening can significantly improve outcomes when preserving natural joints.
Patients who want to protect their mobility long term often look for reliable joint health tips to support their treatment plan. Even simple changes in movement habits and daily routines can reduce wear on vulnerable joints.
How Does Hip Preservation Surgery Work?
Hip preservation surgery focuses on correcting mechanical problems before severe arthritis develops. Instead of replacing the entire joint, surgeons reshape or repair structures inside the hip so the bones move smoothly again.
One common condition treated this way is femoroacetabular impingement, where abnormal bone shapes cause impingement (or a pinch) inside the joint. Surgeons can remove excess bone and restore normal motion through minimally invasive procedures.
Another technique involves repairing the hip labrum, a ring of cartilage that stabilizes the joint. When this structure tears, patients often experience pain and stiffness. Repairing it early can restore stability and prevent further cartilage damage.
These procedures often fall under the broader category of joint preservation treatments because they focus on repairing the natural joint rather than replacing it with artificial components.
Recovery usually includes rehabilitation and carefully guided physical activity. Strengthening the muscles around the hip helps protect the joint during healing and allows patients to return to normal movement patterns.
What Is Regenerative Medicine for Knees?
Regenerative medicine represents one of the most promising directions in modern orthopedic care. Instead of relying solely on surgical correction, doctors use biological therapies to stimulate the body’s natural healing abilities.
Treatments may include platelet-rich plasma injections, stem cell therapies, or specialized biologic materials that support tissue repair. These therapies aim to reduce inflammation and encourage cartilage regeneration within the joint.
For knee injuries or early arthritis, regenerative approaches can help slow degeneration and improve function. This approach fits naturally into broader strategies for preservation of joint space, especially when cartilage damage remains limited.
Many patients exploring these options want to understand how to preserve their joints without immediately resorting to replacement surgery. Regenerative medicine can sometimes extend the lifespan of a natural joint for many years.
While results vary depending on the condition and severity of damage, these treatments often provide meaningful improvements in pain and mobility. When combined with proper rehabilitation and lifestyle adjustments, they can support long-term joint function.
How to Find the Right Joint Preservation Center?
Choosing the right medical provider can make a major difference in treatment outcomes. Joint preservation requires specialized expertise because doctors must identify the precise mechanical or biological issue causing joint degeneration.
A dedicated orthopedic center typically offers advanced imaging, minimally invasive surgical techniques, and regenerative treatment options. This multidisciplinary approach allows physicians to tailor treatment plans to each patient’s unique anatomy.
Facilities such as the Total Joint Center often include specialists who focus specifically on preserving joints whenever possible before considering replacement procedures.
Patients should also look for surgeons experienced in preservation procedures, particularly for hips and knees. The success of these techniques depends heavily on proper diagnosis and precise surgical execution.
It also helps to ask about rehabilitation programs and long-term care strategies. Effective joint preservation doesn’t end with the procedure itself; ongoing therapy, monitoring, and preventive strategies help ensure the joint continues to function well.
Wrap Up
What is joint preservation ultimately comes down to protecting the body’s natural structures whenever possible. Instead of replacing a joint immediately, doctors look for ways to repair damage, restore alignment, and encourage healing so the joint can keep functioning.
For many patients, these strategies provide a meaningful alternative to replacement surgery. With early diagnosis, targeted treatment, and proper rehabilitation, joint preservation can reduce pain, improve mobility, and extend the life of natural joints for years.
If you’re looking to stay active and avoid or delay surgery, joint preservation may offer a powerful path forward—helping you protect your mobility and quality of life with expert guidance from the Orthopedic Institute of NJ.
OINJ PHYSICIAN’S ADVICE
There are a variety of joint preservation treatment options available to delay or ultimately avoid a joint replacement surgery. Biologic injections, such as platelet rich plasma, harness your body‘s natural healing power and are an important part of non-surgical treatment. Surgical options include different cartilage restoration procedures, depending on the size and extent of your cartilage damage. Our skilled joint preservation surgeons at OINJ can help you decide which option is best for you!

Ashley Bassett, MD
Orthopedic Surgeon