

Physicians
Physiatry
Spine (non-operative)
 Healthgrades
Healthgrades
Physiatry
Spine (non-operative)
 Healthgrades
Healthgrades
Orthopedic Surgery
Spine & Neck
 Healthgrades
Healthgrades
PA's, APN-C and LPN's
Body parts
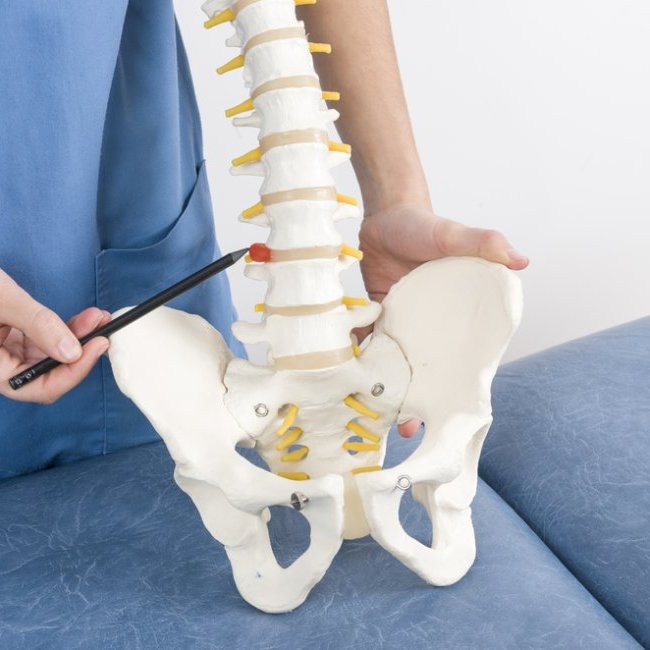
Discs are small, round, filled cushions — almost like shock absorbers — that are found between each of the vertebrae (bones) in your spinal cord. The outside of the discs is tougher than the inside — think of a car’s tire that’s filled with a thick gel. When a disc “bulges,” it means that the disc has for some reason shifted out of position, and the gel-like substance inside it has, correspondingly, shifted position; rather than being evenly spread, it now lists to one side, putting pressure on one of the walls of the disc. When a disc is “herniated,” it means that the fluid inside has found a tiny crack in the tougher outside membrane and has started to leak out. Herniated discs are sometimes referred to as “slipped” or “ruptured.”
You may have a bulging or herniated disc and never know it. What happens sometimes, however, is that the affected disc impinges on a nerve. Most often, this will occur in the lumbar (lower) part of the back, where most of the weight of the upper body comes to bear. Sometimes, it happens in the cervical region, affecting the neck. It can also occur in the thoracic vicinity (in the middle of the back, opposite the chest), where its symptoms can be confused with chest or stomach pain.
If the impingement or pressure is in the lumbar vicinity, you might feel pain, tingling, or numbness in your buttocks or legs; if it is in the cervical region, these symptoms would be experienced in the neck, shoulders, and arms. In severe forms of either case, everyday motions would be difficult, and there might be bowel or bladder issues as well. And in critical cases, the bulging or herniated disc may affect the cauda equina nerve complex at the base of the spine. If this region gets pressured, or squeezed, your legs would be very weak or numb and incontinence can occur.
Discs are subject to the same wear and tear as the rest of the body, so it makes sense that these conditions would arise more as we get older. The discs lose their sponginess, becoming drier and less flexible; a slight injury, or even just the progression of regular motion, can cause a slippage or a tiny tear. Lifting heavy objects improperly — using your back, instead of your legs — can put added pressure on your discs; being overweight can do the same. Your occupation — if it is physical, involves lifting or twisting — can play a role, as does genetics.
“Most cases of pain that stems from a bulging or herniated disc respond well to conservative and non-invasive treatment,” says Christopher Castro DO, a physiatrist at OINJ. “You can try home remedies like over-the-counter pain relievers; simply avoiding positions in which you feel pain; and exercise. When your pain interferes with your daily life, or is constant, we can help. A physical exam will help determine the cause of the pain, and its location.
If the condition is severe, tests that can be done, such as x-rays, CT scans, MRIs, and a myelogram — an x-ray or CT scan that follows the electrical pulses from your nerve as it travels to see its effect on the spine. These can help plan the proper course of action.” There are other classes of medication that might be prescribed. “Anticonvulsants can help with radiating pain,” says Michael Gutkin, MD, another physiatrist at OINJ. “Muscle relaxants can help if your condition is presenting with muscle spasms. There’s also the possibility of oral steroids or a cortisone injection, which can help reduce swelling and inflammation so that your range of movement can improve and you’ll have less pain.” Dr. Gutkin continues, “Physical therapy can help. And if your bulging or herniated disc is affecting the cervical zone, a form of traction could also help: your head is pulled gently away from your neck to allow the bones to reposition. This manipulation gives the small bones in the neck some space to spread.” Surgery is rarely recommended in these cases, but a physical exam and evaluation will lead to the right diagnosis, a prerequisite for finding the best treatment plan.