Search
Find a Physician
Sciatica
Related body part
Physicians & Assistants
What is Sciatica?
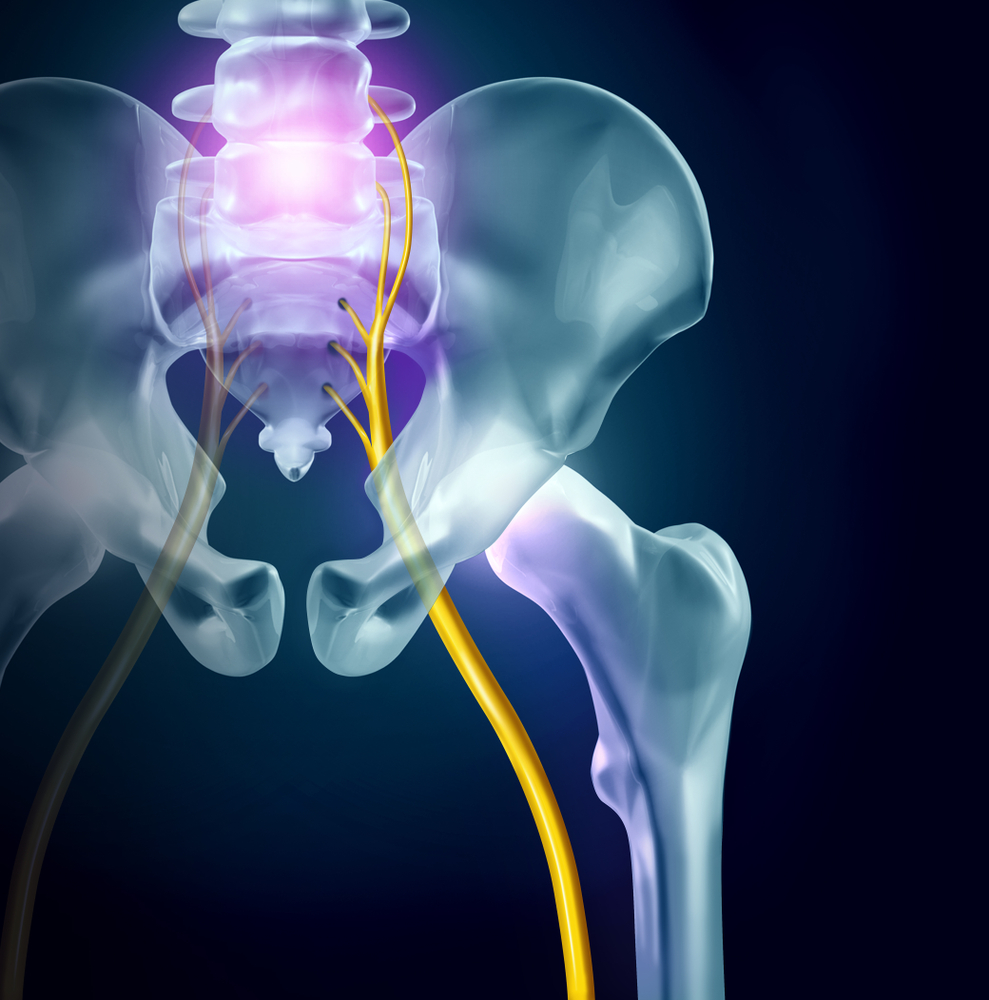
Sciatica--when pain shoots down your leg from your buttocks to your feet--is one of the most common symptoms of lumbar radiculopathy, which is a pinched/compressed nerve at the root of the spinal column. The back pain of sciatica is common. Sciatica/lumbar radiculopathy affects about three million people in the US every year.
Common Causes of Sciatica/Lumbar Radiculopathy:
- A damaged disc can pinch the roots of the sciatic nerve, which starts at the base of your spine, then branches down your left and right buttock and leg. The sciatica nerve is the largest single nerve in the human body.
- Bone spurs or stenosis, a narrowing of the spine as a result of just getting older, can also compress nerve roots in your lower back.
Injury. - Poor posture.
- Pregnancy can lead to looser ligaments in your back and increase pain.
- Obesity; added weight can increase pressure on the spine.
- Sitting for long periods.
- Repeated twisting or lifting.
Symptoms of Sciatica/Lumbar Radiculopathy
- Pain that starts in the lower back and travels down the leg or foot
- Sharp, burning feeling or electric jolt sensation
- Numbness
- Tingling
- Weakness
Back pain doesn’t always warrant a trip to the spine doctor, especially if you know why it’s happening (you went rock climbing, for example). But sciatica does, especially if you have severe symptoms of lumbar radiculopathy, including intense pain, numbness and weakness. See a spine doctor immediately if you experience these symptoms.
Best Treatment for Sciatica/Lumbar Radiculopathy
Your Orthopedic Institute of New Jersey (OINJ) orthopedic spine doctor will do a series of physical tests that involve having you move in different positions, such as walking on your heels and squatting to determine which spinal nerve root is affected.
Your spine doctor will also ask you about positions that make you feel better or worse, the severity of your pain and the length of time you’ve had it.
You may be prescribed anti-inflammatories, muscle relaxants or steroids. These medications can directly provide pain relief. And because the pain is relieved, you may be able to exercise. Being active promotes recovery by helping you get stronger, particular in your core muscles, and more flexible. With this type of non-operative treatment, sciatica/lumbar radiculopathy often resolves within six to twelve weeks.
For severe sciatica/lumbar radiculopathy, your OINJ orthopedic surgeon may order imaging tests, such as an X-ray, MRI, CT scan or a special test, an electromyograph (EMG), which measures the electrical impulses your spinal nerves produce as well as the response of your muscles to those impulses. An EMG test can help your spine doctor make a more informed diagnosis by distinguishing whether spinal nerves are degenerating or being compressed.
Overall, your treatment will depend on the cause of the lumbar radiculopathy. It can range from back supports, medication and physical therapy to steroid injections and surgery. Steroid injections are performed under X-ray guidance to ensure the medication is getting to the appropriate spot.
Surgical Solutions for Lumbar Radiculopathy
Surgical treatment for lumbar radiculopathy depends on what is causing your radiculopathy. If a single degenerated disc is pressing on the nerve root, than isolated removable of that disc (“discectomy”) may be all that is necessary. If your lumbar radiculopathy is being caused by a bony problem, then decompression of the bone by removing part of the lamina, the back of the spinal column, (“hemilaminectomy”) or the entire lamina (“laminectomy”) may be performed. If multiple levels are involved or there is any instability of your spinal column, fusion of the lower back may be necessary.
Healing Advice – Sciatica Fit Tips
OINJ PHYSICIAN’S ADVICE
We look to non-operative solutions first, especially in mild cases of sciatica.

Christopher Castro, DO
DO, OINJ Physiatrist
OINJ PHYSICIAN’S ADVICE
Anti-inflammatories, muscle relaxants or steroids can often provide pain relief for sciatica. And because the pain is relieved, you’ll be better able to complete exercises that will aid in recovery by helping you get stronger and more flexible.

Michael S. Gutkin, MD
DO, OINJ Physiatrist























